Skift Take
As in-person events resume, many options for screening attendees for possible infection are emerging. Each has its pros and cons, and sorting out which is right for your event presents its own challenges. Here, we offer a breakdown of the different methods in terms of cost, accuracy, and scalability.
Thermal cameras have already been introduced at Asian events like the MBC Architecture Show in South Korea, and several industry guidelines have outlined suggestions for testing procedures.
How much protection do these screening methods offer, and how practical are they to implement? Event planners are understandably reluctant to invest in technologies that may offer only limited benefits, particularly when budgets are already strained under the pressure of economic recovery.
We look at some of the most notable screening devices on the market today and weigh the costs against the benefits to give you a clear view of your options and their implications.
Thermal Cameras for Temperature Screening
A fever was one of the first symptoms to be associated with Covid-19, and subsequent data suggests that it is still one of the top symptoms: the CDC estimates that between 83% and 99% of symptomatic patients eventually develop a fever. With that said, many of these patients do not have a fever at the onset of symptoms, and there is still significant concern that presymptomatic cases may be major drivers of transmission. A fever can also be masked by Tylenol and other pain killers, a tactic reportedly used by a since-deceased employee at a Tyson meat-packing plant.
What does all this mean for event planners? Pinpointing fevers among your attendees may be an effective way to identify potential carriers of Covid-19, but it is not a surefire method for catching all potential cases. Still, as long as your efforts don’t create a false sense of security, it makes sense to use whatever risk-management tools are available within your budget.
Thermal cameras have been growing in popularity because they allow a large number of people to be screened simultaneously. These devices typically range in price from $5,000 to $30,000 USD, but some of the more affordable models lack the accuracy required for medical applications. They can be off by as much 5°F (3°C) — or in other words, the difference between a normal temperature and a fever. Even the more advanced cameras are still designed for reading surface skin temperatures, which may not always accurately reflect a person’s core body temperature.
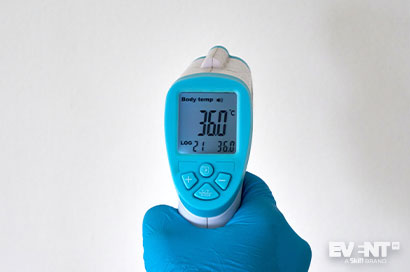
Handheld contactless thermometers provide a more precise way to measure fevers, and they are theoretically less expensive if you disregard the added labor costs. For smaller events, a standard thermometer-based temperature check might be the most cost effective and reliable method for catching fevers. For larger events, the potential bottleneck created by this method may undermine the benefits. It takes time to check each person’s temperature individually, and the last thing you want is long line-ups of people forced into close contact. In such cases, it probably makes sense to use thermal cameras to identify potential fevers, and handheld thermometers to verify them.
It’s also a good idea to check local government regulations around this kind of mass health screening. Speaking to the publishers of the AIPC and UFI Good Practice Guidance, World Forum General Manager Michiel Middendorf explained that their safety team was “already well down the road towards organizing a thermal camera health screening solution when [they] discovered doing so was technically illegal under current Dutch labor and privacy laws.”
Make sure that it’s the right solution for your event before investing heavily in a new technology.
Testing Options
When it comes to on-site testing, there are three major factors to consider: accuracy, cost, and timeliness. In many cases, it may also be necessary to coordinate your efforts with local health authorities.
It may also be most cost-effective to collaborate with an existing lab. While some labs have been charging insurers upwards of $2,000 per test, most prices range within $95 to $209 USD. Many labs also offer results in 24 to 48 hours.
There are also a variety of testing machines available on the market, and they range substantially in terms of cost, speed, and accuracy. Here is some of the relevant information at a glance:
ID Now Machine:
- It produces rapid results (13 minutes or less), but only one sample at a time.
- It self-reports a high level of accuracy, but external reports suggest a high number of false negatives (positive results appear to be more reliable, but this means that potentially infected people could slip through the cracks).
- A pack of 24 testing kits (not including the machine) retails for $2,170.00 USD (or about $90.50 per test).
Cepheid PCR Machine:
- It produces results in 30 to 45 minutes.
- Like the ID Now method, it can process only one sample at a time.
- One model retails for $17,500 USD, not including the cost of testing cartridges.
- Research shows that it has 99.5% accuracy for positive results and 95.8% accuracy for negative results.
Standard RT-PCR Testing Machines:
- Most labs use this technology.
- They generally produce results in about 90 minutes.
- Some PCR machines can process 96 samples at a time (96-well machines retail for around $55,000 USD).
- Other models can process 384 samples at a time (384-well machines retail for around $69,000 USD).
- They generally have a 96% accuracy rate for negative samples and a 100% accuracy rate for positive samples.
- The swabs and tubes/media retail for about $1 USD and $4.70 USD each, respectively; in other words, testing kits should cost under $6 USD each.
QuantLase Laser Blood Test:
- This technology is in its infancy, but the developers claim that it will be available within a few months.
- Using lasers and AI to detect virus-related changes in blood cells, it reportedly produces results within seconds.
- The makers claim that it has an 85% to 90% accuracy rate.
- It is projected to cost as low as $27 USD.
Keep in mind that on-site testing will also involve hiring registered nurses to perform nasal swabs and other tests. In the US, nurses make $35.36 per hour on average.
While new laser technologies may mean significantly faster testing times, the technology that is available right now does not facilitate rapid testing on a large scale (as mentioned before, the “rapid” testing devices are able to process only one test at a time). Rapid testing machines might be reasonable for high-level VIP meetings, but they are not practical for events with a large number of attendees.
For larger events, planners should generally expect to wait at least 24 hours for test results to be processed, although it is theoretically possible to produce them faster with access to more testing machines. Unless you expect attendees to arrive a day in advance and remain isolated until results are returned, it may make sense to limit testing only to individuals who display other risk factors like a fever, or just to members of staff.
Very large-scale events with big budgets might consider purchasing testing machines themselves, but for small events, it probably makes more sense to coordinate testing efforts with local lab facilities. Venues may also find it worthwhile to invest in testing solutions as they can spread the investment over more events, in which case it may become a competitive lever.
IN CONCLUSION
There are many tools available to help event planners screen attendees and staff for Covid-19 infections, but no solution offers any guarantees. Generally, the more accuracy that a screening method provides, the more costly and time-consuming it is.
Here’s a review of the main factors to consider:
- Thermal cameras provide rapid mass-screening of attendees for fevers, but they may have issues with accuracy and present conflicts with privacy regulations.
- Handheld thermometers require more staff and longer screening times, but offer greater accuracy and lower upfront costs.
- Rapid Covid-19 tests that are on the market now can only process one sample at a time, and the fastest models seem prone to false negatives.
- Slower RT-PCR Covid-19 testing devices can process up to 384 samples at a time, so they are the most time-efficient option for large-scale events (most labs use this method).
- Major event producers may wish to invest in their own PCR testing machines, but planners operating on a smaller scale will likely want to partner with existing labs.
- Different regions may have regulations around who can perform Covid-19 tests. Check with your local authorities before investing in a testing initiative.
- New testing methods may offer faster and cheaper options, but they are still in their infancy.
While screening for Covid-19 may present multiple logistical challenges at this time, the technology is continually advancing. We already have some useful tools at our disposal, and more are being developed as we speak.